A trauma bond is a strong emotional attachment that forms in an abusive relationship. It develops through repeated cycles of harm followed by affection, apology, or calm.
It has nothing to do with weakness.
If you’ve felt unable to leave someone who hurts you, or found yourself defending them to others, this is worth exploring. The pattern has a name and an explanation.
For LGBTQIA+ individuals, affirming mental health treatment can make a real difference. Especially when identity, past healthcare experiences, and community dynamics all factor into how safe it feels to ask for help.
Need to Know
- A trauma bond forms through cycles of abuse and intermittent affection, not personal failure.
- The brain’s own chemistry makes these bonds genuinely hard to break.
- Childhood trauma and early attachment experiences can increase vulnerability.
- LGBTQIA+ individuals may face added barriers to leaving due to minority stress or lack of affirming support.
- With the right support, healing is possible.
What Makes a Trauma Bond Different From a Difficult Relationship?
Not every painful relationship is a trauma bond. Two things set it apart: a significant power imbalance and intermittent abuse.
Intermittent abuse means the harm is unpredictable. It cycles with moments of calm, affection, or apology, which is exactly what makes it so disorienting.
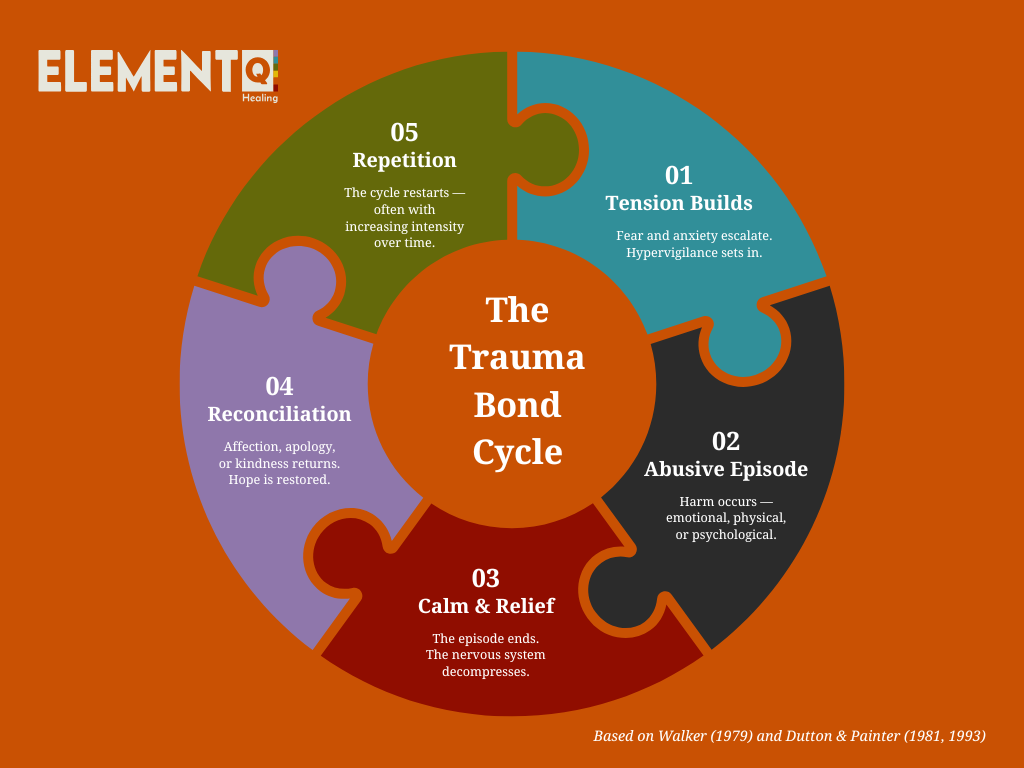
Research by Dutton and Painter found that these two dynamics were the strongest predictors of continued emotional attachment to an abusive partner, even after the relationship ended. [1]
The relief after an abusive episode isn’t a sign that things are improving. It’s the mechanism that keeps the cycle going.
What About Bonds That Form Through Shared Trauma or Substance Use?
You may have heard “trauma bonding” used to describe closeness that forms when two people go through something intense together. That’s a real and distinct experience, and it’s worth taking seriously too.
Relationships that form or deepen through shared substance use or high-intensity experiences can feel profound. That intensity is real. But it can also make it harder to see clearly whether the relationship itself is healthy.
If you’re questioning a relationship that formed this way, you don’t need to have it all figured out right now.
Focusing on your own well-being first is a good starting point. LGBTQIA+-affirming treatment can help you find clarity at your own pace, without pressure to make any decisions about the relationship before you’re ready.
Why Is It So Hard to Leave a Trauma Bond?
The answer isn’t weakness. It’s neuroscience.
When we form close attachments, the brain releases a mix of chemicals that drive bonding and connection. In an abusive relationship, these systems become dysregulated. [2]
Here’s what’s happening neurochemically:
- Oxytocin builds trust and attachment, even toward someone causing harm
- Dopamine drives craving and the urge to seek the other person out
- Endogenous opioids regulate pleasure and pain, and create a cycle of withdrawal when the person is absent
- Cortisol and stress hormones keep the nervous system in a chronic state of activation
After an abusive episode ends, the body experiences relief. The brain begins to associate the abuser with that relief, and unconsciously seeks it again. [2]
This is sometimes called “trauma addiction.” It’s physiological, not a character flaw.
What Are the Signs You Might Be in a Trauma Bond?
Trauma bonds develop gradually. Signs are often subtle at first. Common experiences include:
- Feeling like you’re constantly “walking on eggshells.”
- Blaming yourself when your partner becomes abusive or withdrawn
- Defending or rationalizing their behavior to people close to you
- Feeling physically anxious or activated just by being around them
- Believing you couldn’t survive, emotionally or practically, without them
- Intense cycles of closeness followed by distance or cruelty
- Knowing the relationship is harmful, but feeling unable to leave
You don’t need to check every box. One or two of these is worth paying attention to.
How Does Childhood Trauma Shape Trauma Bonding in Adulthood?
Childhood experiences shape the nervous system in lasting ways.
When caregivers are both a source of harm and comfort, the brain adapts. It learns to associate love with unpredictability, and fear with closeness.
Psychologist Bessel van der Kolk found that people exposed to childhood violence or neglect begin to expect these dynamics as a normal part of relationships. [3]
Over time, chronic stress alters brain structures involved in memory, emotional regulation, and threat response. [3] These changes aren’t flaws. They’re survival adaptations.
In adulthood, trauma bonds can feel familiar because of this, which is part of why they’re so hard to recognize from the inside.
Stockholm Syndrome follows the same mechanism: attachment that forms toward an abuser as a protective psychological response. It’s trauma bonding in a different context.
What Does Healing From A Trauma Bond Actually Look Like?
Healing is possible. Research supports this fact.
A study by Dutton and Painter found that emotional attachment to an abusive former partner decreased by around 27% within six months of separation. [1] Distance and time genuinely shift the bond.
Support accelerates that process.
Reducing or ending contact is often necessary, though rarely simple. Trauma-focused therapy helps address the neurological roots of the bond, not just the surface behaviors.
Approaches that can help include:
- EMDR
- Somatic therapy
- Internal Family Systems (IFS)
- Cognitive Processing Therapy (CPT)
- Attachment-based therapy
For LGBTQIA+ individuals, care that understands how identity and minority stress intersect with trauma bonding makes the process feel safer. You shouldn’t have to explain or defend who you are to get support.

Ready to Start Building Healthier Relationships?
Healing from a trauma bond isn’t just about leaving a relationship. It’s about coming back to yourself. Learning what safety feels like. Building connections that don’t cost you your sense of self.
There’s no timeline you have to follow.
If you’re ready to explore what support could look like, we’re here.
Verify your insurance or give us a call at 858-422-1860.
Frequently Asked Questions
1. How do you know if you are trauma-bonded?
Common signs include feeling unable to leave despite knowing the relationship is harmful, blaming yourself for your partner’s behavior, and feeling physically anxious around them. You might also notice your sense of self becoming tied to the relationship, or find yourself defending someone who consistently hurts you. A trauma-informed therapist can help you make sense of what you’re experiencing.
2. What are the 7 stages of the trauma bond?
The seven stages are: love bombing (intense idealization), gaining trust, criticism (subtle devaluation begins), manipulation (gaslighting and control), resignation (self-blame sets in), distress (leaving feels impossible), and repetition (the cycle restarts). Most people don’t recognize these stages while they’re inside them, which is part of what makes trauma bonds so difficult to name.
3. How does a trauma bond work?
A trauma bond forms through intermittent reinforcement, cycles of harm followed by relief or affection. The brain begins to associate the abusive person with relief from distress, creating a neurochemical pull that feels compulsive. This happens even when someone logically understands the relationship is harmful.
4. Does a trauma bond ever go away?
Yes. Research shows attachment to an abusive former partner decreases meaningfully in the months after separation. [1] Trauma-focused therapy, distance from the abusive person, and rebuilding a sense of self all support that process. Healing isn’t always linear, but it is possible.
5. Can therapy help break a trauma bond?
Yes. And it’s often essential. Approaches like EMDR, somatic therapy, IFS, and Cognitive Processing Therapy address the neurological patterns underneath the bond. For LGBTQIA+ individuals, working with affirming providers who understand community-specific dynamics makes the process feel safer and more sustainable.






