If you’ve ever wondered how long alcohol stays in your system, the short answer is: it depends.
Most standard tests can detect alcohol anywhere from a few hours to up to 90 days after your last drink. The type of test matters, and so does your body.
This article will walk you through what the research actually shows.Navigating questions about alcohol use? Element Q offers affirming, trauma-informed support for the LGBTQIA+ community in San Diego.
Need to Know
- Alcohol is detectable in blood for up to 12 hours, in urine for up to 72 hours or more after heavier use, and in hair for several months.[1]
- Your liver processes roughly one standard drink per hour, though this varies from person to person.[2]
- Drinking water, coffee, or sleeping does not speed up alcohol clearance.
- Age, weight, food intake, metabolism, and medications all affect how long alcohol stays in your system.
- If alcohol use has started to concern you, affirming support exists, and reaching out is a valid next step.
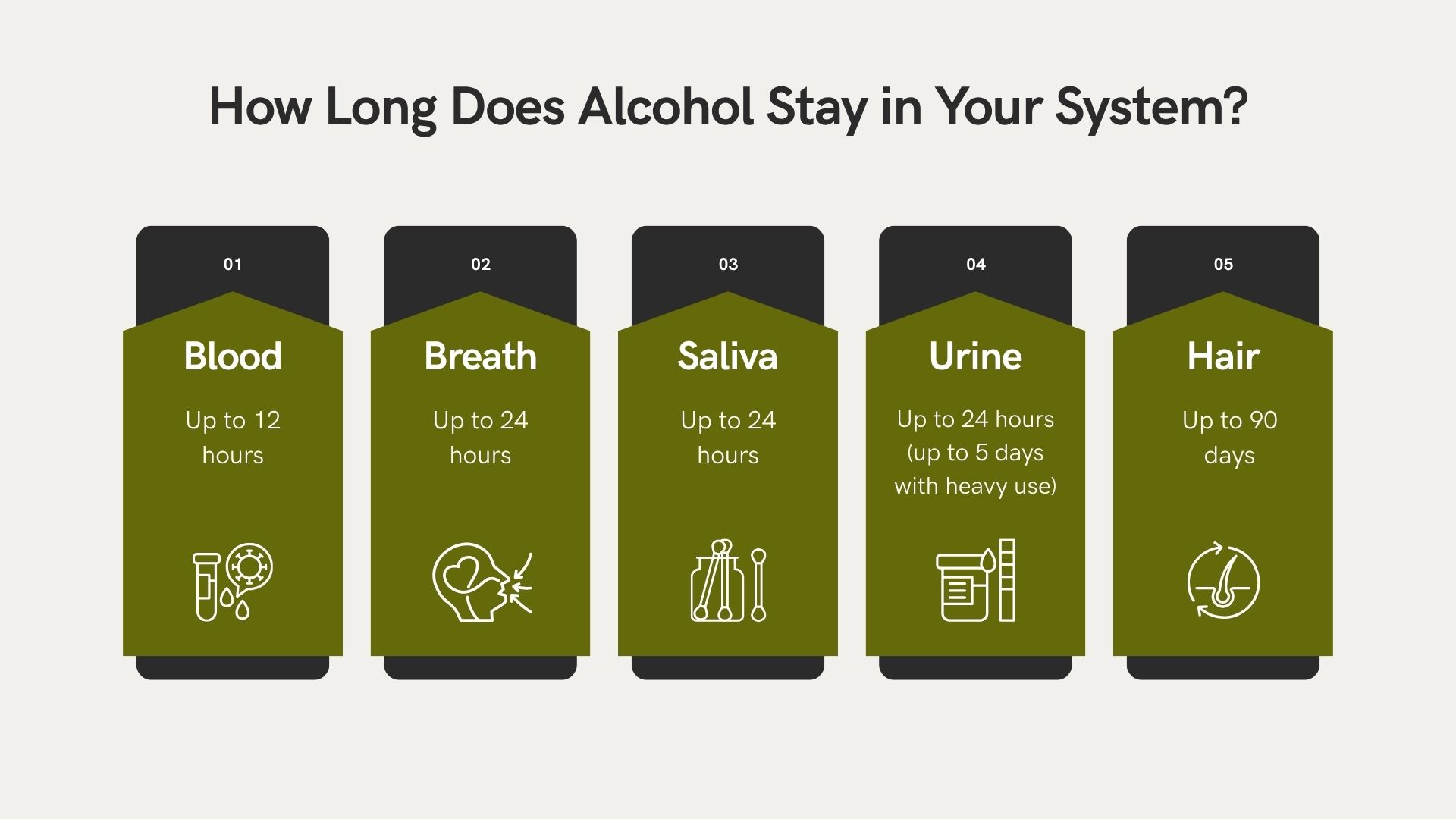
How Long Does Alcohol Stay in Your System, Exactly?
Detection windows vary significantly depending on the type of test being used. Here’s what the research shows:
- Blood: Up to 10 to 12 hours [1]
- Breath: Typically detectable for up to 24 hours, depending on the amount consumed
- Urine: Up to 24 hours with standard testing; 72 hours or more after heavier use[1]
- Saliva: Mirrors blood alcohol concentration; detectable within hours of drinking
- Hair: Several months, based on a 3 to 6 cm proximal hair segment[1]
Detection doesn’t necessarily equal impairment. Alcohol can still appear on a test well after the effects have worn off, which is why the type of test matters depending on the context.
How Does Your Body Process Alcohol?
Your liver does most of the work.
When you drink, alcohol is absorbed directly into the bloodstream through the stomach lining and upper small intestine. It reaches the brain almost immediately. [2]
From there, an enzyme called alcohol dehydrogenase breaks it down at an average rate of 15 to 25 milligrams per hour. [2]
A small amount, roughly 2 to 5%, also leaves the body through sweat, breath, and urine. [4]
Eating before or while drinking slows absorption. It doesn’t stop it, but it gives your liver more time to keep up.
What Factors Affect How Fast Alcohol Leaves Your System?
No two people process alcohol at the same rate. Several variables shift your clearance timeline:
- Age. Metabolism tends to slow over time
- Body weight and composition. Alcohol distributes differently based on size and fat-to-muscle ratio
- Biological sex. Bodies with higher water composition dilute alcohol more effectively
- Metabolism. Individual metabolic rate plays a significant role
- Food intake. Eating slows absorption into the bloodstream
- Type and strength of alcohol. Higher ABV means more alcohol per serving
- Medications. Some affect how alcohol is metabolized or intensify its effects
A standard drink is 12 oz of regular beer, 5 oz of wine, or 1.5 oz of distilled spirits. [3] Drinking multiple standard drinks in a short window outpaces what the liver can process, causing BAC to climb.
Does Drinking Water or Coffee Help You Sober Up Faster?
No. This is one of the most persistent myths about alcohol.
Water, coffee, a cold shower, or sleep will not speed up how fast your liver processes alcohol. [4] They may help you feel more alert or comfortable, but they don’t change your BAC.
Time is the only thing that clears alcohol from your system.
This matters practically. Feeling better doesn’t mean you’re safe to drive, take medication, or make important decisions. Impairment can persist even when it’s no longer obvious.
What Does Alcohol Feel Like at Different BAC Levels?
BAC rises as you drink, and the effects shift at each threshold.
Most people begin noticing effects around 0.05% BAC. At 0.10%, clear signs of intoxication are typically present. [4][5]
Common signs include:
- Lowered inhibitions
- Slurred speech
- Impaired coordination
- Difficulty concentrating or remembering
- Slower reaction time
- Nausea or vomiting at higher levels
People with higher tolerance may not feel as impaired at the same BAC. But impairment is still real and still measurable.
Feeling in control isn’t the same as being in control.
What Happens When You Mix Alcohol With Medications?
Alcohol doesn’t interact the same way with every substance. Some combinations carry serious risks.
Alcohol and SSRIs
Mixing alcohol with antidepressants can intensify sedation, impair judgment, and work against the stability your medication is building. The combination affects people differently depending on the type of antidepressant prescribed.
Some people notice increased anxiety or emotional dysregulation when combining alcohol with their medication. Others may find that their antidepressant becomes less effective over time.
Antidepressants like SSRIs are commonly prescribed for depression and anxiety, conditions that affect LGBTQIA+ individuals at higher rates due to minority stress and discrimination. If you’re taking an antidepressant and have questions about alcohol, your prescribing provider is the right person to ask.
Alcohol and Opioids or Sedatives
This combination is particularly dangerous.
Both alcohol and opioids suppress the central nervous system, including breathing. Together, even moderate amounts of alcohol can significantly increase overdose risk. [5]
This is one of the most common factors in alcohol-related emergencies.
When Does Alcohol Use Become Worth Paying Attention To?
It doesn’t have to reach a crisis point to be worth examining.
According to SAMHSA, roughly 29.5 million people aged 12 and older met criteria for alcohol use disorder in 2021. [6] LGBTQIA+ individuals face elevated rates of alcohol use, often tied to minority stress, discrimination, and limited access to care that understands their experiences. [7]
If alcohol has started affecting your sleep, relationships, mental health, or daily functioning, that’s enough.
You don’t have to be in crisis to deserve support. Identity-affirming outpatient programs, including IOP and PHP, offer structured help without requiring you to step away from your life. If you’re curious about what that looks like, our page on affirming dual diagnosis treatment has more context.

How Element Q Can Help
If alcohol use is something you or someone you care about has been navigating, you don’t have to figure it out alone.
Element Q offers PHP and IOP programs designed specifically for LGBTQIA+ individuals in San Diego. Our clinicians bring both lived experience and advanced clinical training to treatment, addressing the root causes of alcohol use, including trauma, minority stress, and dual diagnosis.
Substance use treatment includes individual therapy, group sessions, psychiatric support, and holistic healing—all in an affirming space where you won’t have to explain who you are.
Call us at 858-422-1860 or let us verify your insurance to take the next step.
Frequently Asked Questions
1. How long does it take for alcohol to fully be out of your body?
It depends on how much you drank, your metabolism, and what type of test is being used. Standard blood tests can detect alcohol for up to 12 hours after your last drink. Urine tests typically detect alcohol for up to 24 hours, and up to 72 hours or more after heavier use. Hair testing can reflect alcohol use over a period of several months.
2. Does drinking water flush out alcohol?
No. Water does not lower your BAC or speed up how fast your liver processes alcohol. It can help prevent dehydration, which is a common side effect of drinking, but it won’t clear alcohol from your system faster. Only time does that. Drinking large amounts of water before a urine test may dilute the sample, but it won’t eliminate alcohol from the results.
3. Can you still be drunk after 7 hours?
Yes, depending on how much you drank. At an average metabolism rate of roughly one standard drink per hour, someone who had six or seven drinks could still have a measurable BAC well past seven hours. Tolerance can mask the feeling of impairment without actually reducing it. Feeling sober and being sober are not always the same thing.
4. What happens if you drink alcohol on SSRIs?
Mixing alcohol with SSRIs can intensify sedation, worsen mood symptoms, and reduce the effectiveness of your medication over time. Alcohol is a depressant, and it can work directly against what your antidepressant is trying to do. Some people also experience increased emotional dysregulation or anxiety when combining the two. If you’re on an SSRI and wondering whether it’s safe to drink, that’s a conversation worth having with your prescribing provider.
4. What is a standard drink, and why does it matter?
A standard drink in the United States contains about 14 grams of pure alcohol, equivalent to 12 oz of regular beer, 5 oz of wine, or 1.5 oz of distilled spirits. Understanding what counts as a standard drink matters because BAC and clearance time are directly tied to how much alcohol you actually consumed. Portion sizes in real life often exceed standard drink definitions, which means many people underestimate how much they’ve had.
Sources
[1] Andresen-Streichert, H., Müller, A., Glahn, A., Skopp, G., & Sterneck, M. (2018). Alcohol biomarkers in clinical and forensic contexts. Deutsches Arzteblatt International, 115(18), 309–315. https://doi.org/10.3238/arztebl.2018.0309
[2] Norberg, Å., Jones, A. W., Hahn, R. G., & Gabrielsson, J. L. (2003). Role of variability in explaining ethanol pharmacokinetics: Research and forensic applications. Clinical Pharmacokinetics, 42(1), 1–31. https://doi.org/10.2165/00003088-200342010-00001
[3] National Institute on Alcohol Abuse and Alcoholism. (n.d.). What is a standard drink? U.S. Department of Health and Human Services. https://www.niaaa.nih.gov/alcohols-effects-health/overview-alcohol-consumption/what-standard-drink
[4] Paton A. (2005). Alcohol in the body. BMJ (Clinical research ed.), 330(7482), 85–87. https://doi.org/10.1136/bmj.330.7482.85
[5] National Institute on Alcohol Abuse and Alcoholism. (2018). Understanding the dangers of alcohol overdose. U.S. Department of Health and Human Services. https://www.niaaa.nih.gov/publications/brochures-and-fact-sheets/understanding-dangers-of-alcohol-overdose
[6] Substance Abuse and Mental Health Services Administration. (2022). 2021 National Survey on Drug Use and Health: Key substance use and mental health indicators in the United States. U.S. Department of Health and Human Services. https://www.samhsa.gov/data/sites/default/files/reports/rpt39443/2021NSDUHFFRRev010323.pdf
[7] Zollweg, S. S., Belloir, J. A., Drabble, L. A., Everett, B., Taylor, J. Y., & Hughes, T. L. (2023). Structural stigma and alcohol use among sexual and gender minority adults: A systematic review. Drug and alcohol dependence reports, 8, 100185. https://doi.org/10.1016/j.dadr.2023.100185






